Have you ever bought the wrong tool for a task, only to use it for another purpose later? Using a previously developed drug for another purpose is known as drug repositioning. Drugs on the market today can have unforeseen and even unrelated effects on our bodies, with some proving their real worth as repurposed drugs many years after being developed. This article takes a look at AZT, Viagra and more recently remdesivir as examples of drug repositioning and how this strategy can help develop new medicines.
Drug repositioning (or repurposing) uses old drugs to target new diseases. When drugs are developed, molecules are screened for their activity against a certain disease. However, there is a chance that the drug can work against other diseases too. Examples of successfully repositioned drugs include AZT (cancer to HIV treatement) and Viagra (chest pains to erectile dysfunction).
Old Drugs as New Therapies
When developing new therapies, researchers first identify a specific target to design a drug for. This can be to inhibit pain receptors in our body, for example, or to attack bacterial cell components. They then identify leads (potential drug candidates) using structure-based design to create molecules that they think will affect these targets best. These molecules are then ushered down the drug development process until the final iteration is approved as a new therapy.
In an ideal world, a drug would interact with its intended target and the target alone, but this isn’t the case. Due to the complexity of the human body, many of these drugs often have unintended outcomes, known as side effects. Some common side effects include nausea, headaches and drowsiness; they are listed in the prescription or label as a precaution for the patients.
However, some of these side effects include the ability to target a completely different disease altogether! Due to time and cost restraints, drugs are usually tested in clinical trials for their effectiveness against a single disease or disorder, sometimes several related ones. It can therefore take years for their therapeutic effects against unrelated diseases to surface, often through patient feedback. AZT for HIV and Viagra for erectile dysfunction are two classic examples of drug repositioning.
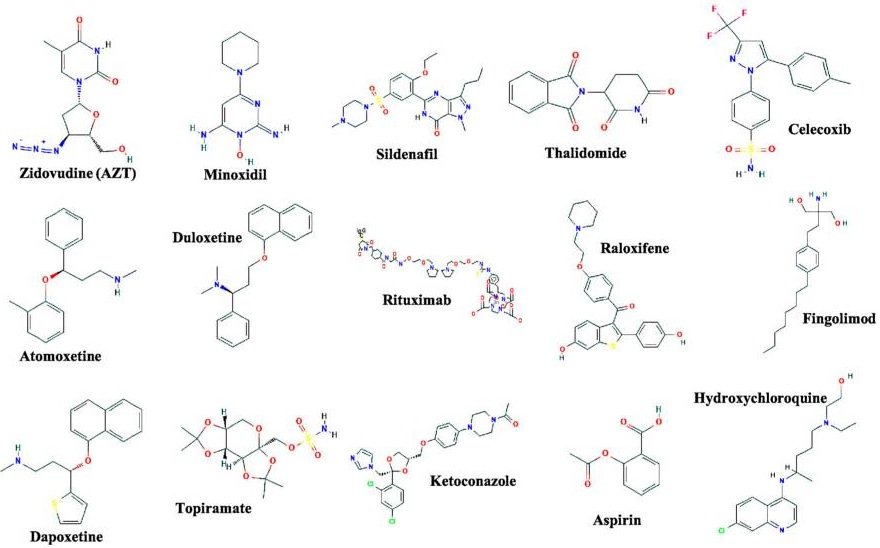
Drug Repositioning Examples
AZT: Failed Anticancer Drug to Life-Saving HIV Therapy
In 1964, azidothymidine (AZT) was created and lauded as a potential anticancer agent. It failed terribly in preclinical trials when mice models showed no anticancer activity. The project was shelved indefinitely, with the research group promptly moving on to the next drug candidate. AZT was forgotten for almost 20 years until the HIV (Human Immunodeficiency Virus) pandemic terrorized the world in the 1980s, leading to AIDS (acquired immunodeficiency syndrome) in patients—for which there was no known cure.
Driven by the urgent need to discover an effective therapy for HIV, existing drugs and old drug candidates were screened for their effectiveness against the retrovirus. If any of these turned out to be viable, it would shorten the time it took for patients to receive treatment, as these potential drugs would be further along the drug development process than if a new compound was to be synthesized from scratch.
AZT was one of these candidate molecules submitted for testing, quickly proving to be highly effective in suppressing HIV activity. It was approved as a drug just 25 months later, in the first successful case of drug repositioning. At the time, it was a miracle drug that prolonged the lives of HIV patients, buying them the time needed for more HIV therapies to become available.
Viagra for Chest Pains?
Many of you will be familiar with Pfizer’s famous diamond-shaped blue pill for erectile dysfunction, but did you know it was created to treat chest pain (angina) and hypertension? In 1993, the drug was ready for clinical trials despite showing limited effectiveness in preclinical data. It was administered to a group of healthy male volunteers in Phase 1 trials, who later returned home to their partners and reported having sustained erections.
Fast forward to 1998, and Pfizer had a blockbuster drug on their hands in the form of Viagra, with men everywhere clamoring for a prescription; it was the first and only oral medication for erectile dysfunction. Viagra generated nearly US$2 billion in annual revenue at its peak and is widely epitomized as the most successful case of drug repositioning in history.
Drug Repositioning as a Research Strategy
The potential of existing drugs to have other therapeutic benefits means drug repositioning is a viable strategy for producing new drugs. Pharmaceutical companies continually test their pool of existing drugs and drug candidates for activity against other diseases. This has several advantages, including accelerating drug development, having stockpiles and existing manufacturing infrastructure.
Repurposing Drugs for COVID-19
The SARS-CoV-2 pandemic sparked the race for a cure to the virus, and many pharmaceutical companies quickly dug up their libraries of existing drugs to study their potential for antiviral activity. Chloroquine and hydroxychloroquine were among the first drugs studied, both FDA-approved medicines used to treat malaria. Despite apparent early success in clinical trials and FDA approval for treating COVID-19, this was quickly overturned by further studies. The initially published papers have since been retracted.
At the time of writing, remdesivir is the only FDA-approved drug for COVID-19, which Gilead Sciences originally developed in 2009 to treat hepatitis C—a virus that attacks the liver. Despite showing no activity against the hepatitis C virus, the company continued to study the drug candidate against Ebola and other viruses. When coronavirus reared its ugly head in early 2020, remdesivir was tested and found effective in improving the recovery rates of COVID-19 patients. By October 2020, the drug was approved by the FDA and sold as Veklury; another successful example of drug repositioning.
There is currently a range of drugs being screened for their effectiveness against the coronavirus, from HIV therapies to corticosteroids to vitamin C. As we learn more about the virus, more targeted repurposing with other drug classes (such as monoclonal antibodies) will be possible.
Patent and Innovation Issues
As with all commercial research ventures, intellectual property rights come to the fore. In normal drug development, patent protection and market exclusivity (the right to sell the drug) are granted to the pharmaceutical company that discovered the drug when it is approved. Therefore, any new treatment possibilities for existing drugs legally belong to the original pharmaceutical company, even if someone else uncovers the activity. As a result, such research is often limited, as it makes financial sense for companies to only screen compounds for which they hold intellectual property rights.
To bypass patent-related issues, pharmaceutical companies often use the ‘me-too’ approach for developing new drugs. Me-too drug design is closely related to drug repurposing, where minor alterations are made to existing drugs to create a (hopefully) better drug. Just like drug repositioning, me-too drugs can sometimes have effects that are unrelated to their parent molecule. The controversy surrounding such strategies is their supposed lack of real innovation since they are less likely to uncover new and novel therapeutic pathways.
The examples of drug repositioning highlighted in this article show that the strategy has its place in the drug development landscape. As seen in the HIV pandemic in the 1980s and the more recent coronavirus, we can produce therapies quickly by repurposing old ones. The collaboration between companies and governments provides essential lessons, showing that we can develop cures for pressing diseases if we pool our resources together and work toward a common goal.
About the Author

Sean is a consultant for clients in the pharmaceutical industry and is an associate lecturer at La Trobe University, where unfortunate undergrads are subject to his ramblings on chemistry and pharmacology.